By: Dr. Samantha Rawdin Over the past few years, medications like Ozempic, Wegovy, Mounjaro, and other GLP-1 receptor agonists have become widely known for their effectiveness in treating type 2 […]
By: Dr. Andrew Koenigsberg That sharp zing when you sip something cold? It’s more common in summer than you think. Summer brings sunshine, iced drinks, and sweet treats — but […]
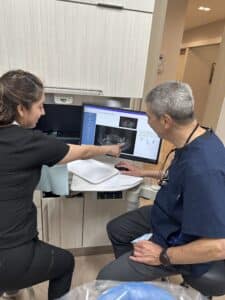
By: Dr. Andrew Koenigsberg Communication is a two-way street, and it is important for both you as the patient and me as your dentist to explain our concerns and expectations […]
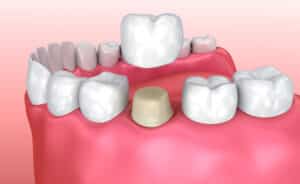
At Gallery57 Dental in NYC, our skilled dental professionals leverage advanced CEREC technology to provide same-day ceramic crowns, transforming patient experiences through precision, convenience, and exceptional results. However, patients often wonder how these […]
Dental anxiety is a common phenomenon that prevents many people from receiving the care they need to maintain a healthy smile. Avoiding dental visits can lead to serious oral health issues, […]
By: Dr. Samantha Rawdin February is American Heart Month and what better way to celebrate than by promoting healthy oral habits that can aid in reducing your risk of cardiovascular […]
Temporomandibular joint (TMJ) disorder, also referred to as temporomandibular dysfunction (TMD), can disrupt your life with pain, discomfort, and difficulty performing everyday activities like eating or speaking. At Gallery 57 […]
By: Dr. Rebecca Koenigsberg What’s the Buzz About Fluoridated Water and IQ? A recent report has raised important questions about a possible link between fluoridated water and lower IQ in […]
By: Dr. Andrew Koenigsberg Introduction: The Shift in Pain Management for Wisdom Teeth Extraction and other Dental Procedures A recent study has confirmed that a combination of acetaminophen (Tylenol) and […]
Teeth stains are a common concern for people who wish to have a brighter, healthier-looking smile. However, not all stains are created equal. Understanding the different types of discoloration and […]